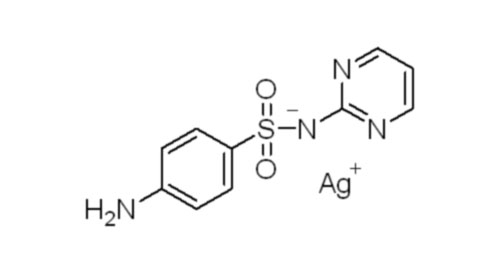
治疗烧伤创面不宜使用磺胺嘧啶银(SSD)
The use of silver sulfadiazine should be discouraged for burn wounds
数十年来,含银抗菌剂一直作为非全层皮肤烧伤患者的标准局部疗法使用。尤其是磺胺嘧啶银(SSD)被普遍用于治疗烧伤。然而,其疗效一直不明确。最近发表的两篇系统评述[1, 2]文章揭示了含银敷料和局部治疗药物治疗烧伤缺乏有效证据。
Silver-containing antibiotics have been applied as standard topical therapy for patients with partial-thickness burns for decades. Silver sulfadiazine (SSD or SD-Ag) in particular is commonly used to manage burns. However, evidence of their effectiveness remains poorly defined. Two recently published systematic reviews [1, 2] suggested the lack of evidence of effectiveness for silver-containing dressings and topical agents in burns.
第一篇系统评述[1]是在英国外科杂志上发表的,Brölmann等人筛选了Cochrane创伤与外周血管疾病组截止到2011年6月发表的所有Cochrane系统评述文章[3]。他们鉴别和审阅了包含109条基于证据的结论的共44篇相关评述。在其文章表2中列出了数条与烧伤有关的证据,包括“其他纤维敷料和含银抗菌剂可能没有效果或甚至延缓了愈合”,“与SSD相比,局部负压治疗5天时烧伤伤口面积缩小”以及“使用SSD霜增加或减少感染率证据有限,相互矛盾。没有证据表明在创伤愈合和伤口感染时局部使用银制剂有效”,同时在对急性创伤(含烧伤)的总结中得出结论“由于多个临床试验显示延缓创伤愈合和增加疼痛及感染率的趋势,磺胺嘧啶银不宜用于烧伤”。而且,在其表8中他们建议“在急性创伤中不要使用磺胺嘧啶银作为局部治疗药物”。
In the first article, published on British Journal of Surgery [1], Brölmann et al. have screened all Cochrane systematic reviews [3] up to June 2011 published by the Cochrane Wounds and Peripheral Vascular Diseases Groups. They identified and reviewed 44 relevant reviews containing 109 evidence based conclusions. Several evidences regarding burns were listed in table 2 of their article, including “Other fibre dressings and antimicrobial (silver) dressings may have no effect on, or even prolong, healing”, “A reduction in burn size at day 5 was seen when TNP (topical negative pressure) was compared with SSD” and “Contradictory limited evidence of increased and decreased infection rates when using SSD cream. No evidence for effectiveness of topical silver for preventing wound infection in terms of wound healing and wound infection”, and they concluded that “For burn wounds the use of silver sulfadiazine should be discouraged, as several trials showed a trend towards wound healing delay and increased pain and infection rates” in their results for acute wounds. Furthermore, they recommended that “In acute wounds do not use silver sulfadiazine as topical agent” in table 8 of their article.
Brölmann引用的一篇系统评述[4]总结了来自治疗浅表烧伤和非全层皮肤烧伤的26项随机对照临床试验的最好证据,结果显示烧伤敷料用水凝胶、硅衣敷料、生物合成敷料和抗菌敷料要比用SSD或洗必泰药纱敷料伤口愈合的更快。这篇评述还发现,虽然在所有相关研究中没有统计意义上的差别,但是有个一致的趋势,就是与SSD或洗必泰敷料相比,使用其他所有干预敷料时病人经受的疼痛更少。
One systematic review [4] cited by Brölmann summarized the best available evidence from a total of 26 included randomised controlled trials (RCTs) relating to the effects of dressings used to treat adults with superficial or partial thickness burns, and the results indicated that burn wounds dressed with hydrogels, silicon coated dressings, biosynthetic dressings and anti microbial dressings healed more rapidly than those dressed with SSD or chlorhexidine impregnated gauze dressings. Also in this review, there was a finding, not statistically significant in all studies but was consistent for all intervention dressings, that the pain experienced by patients appeared to be reduced with the use of the intervention dressing when compared against SSD or chlorhexidine dressings.
如果本文对您有帮助,欢迎使用左边赞赏~
¥赞赏
不错,不错,看看了!